This post is also available in:
Dr. Hannes Schwenke and his team are 3D printing artery models to get a closer look at patient anatomy and ease patient anxiety. Learn more about their process in this article.

Ten years ago, you wouldn’t have believed us if we told you that 3D printing would eventually become affordable enough for doctors to use in their daily practices. A prime example of this exciting new reality is how Dr. Hannes Schwenke uses 3D printing in conjunction with scanning to produce accurate models of patient organs to treat them more effectively.
Dr. Schwenke is a pioneer in the neurosurgeon field. Thanks to 3D printing technology, he and his team at the University Hospital Schleswig-Holstein in Lübeckcon have been able to improve the quality of operations performed on brain aneurysms. Essentially, they 3D print their patients’ brain arteries to prepare for upcoming surgeries. The 3D models help them visualize the situation at hand so they can begin the surgeries with as much prior knowledge as possible.
“The aneurysm surgeries that we do are minimally invasive endovascular procedures through the inguinal arteries or the wrist arteries, all under fluoroscopy,” he explains. “We then access the brain through these approaches with catheters. The skull does not have to be opened.”
From molecules to scale model
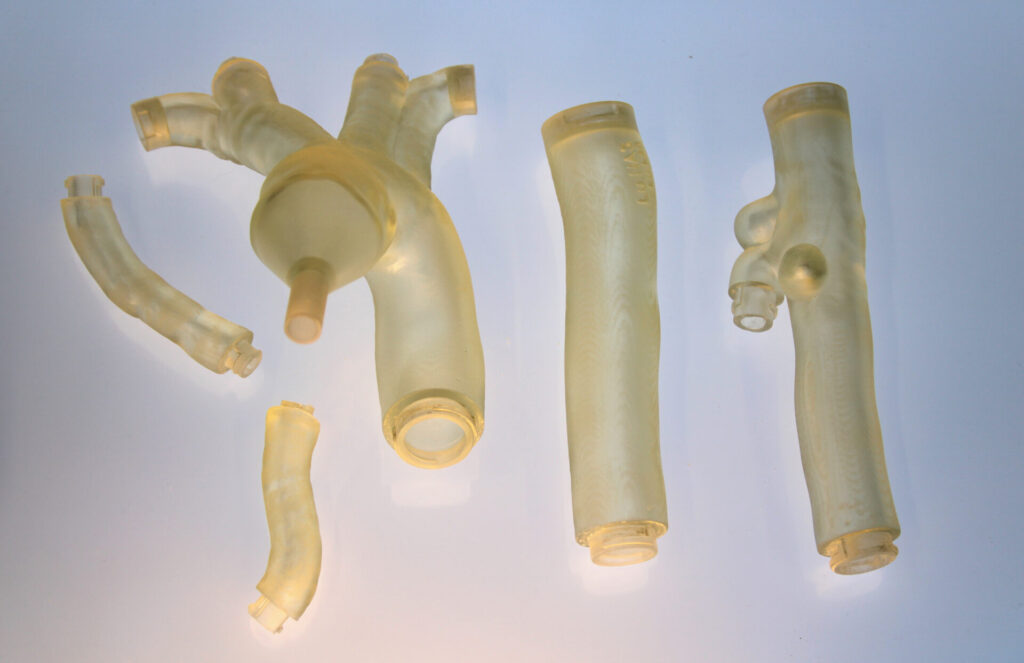
Dr. Schwenke can isolate a relevant artery through a combination of CT scans and 3D rotational angiography (or 3DRA). He started using Netfabb, Fusion 360, and Formlabs SLA hardware about five years ago to create simple brain artery prints using the isolated data.
First, Dr. Schwenke and his team process and prep the data in Netfabb. Then, they carry the data over to Fusion 360 where they design mechanical interfaces. From Fusion 360, the data then becomes a physical, 3D printed scale model of the artery that the team can analyze and even run a fluid dynamic simulation on.
This process minimizes the risks that come with complex brain surgery and saves time, enabling the team to see more patients. The physical models also help him visualize his patients’ anatomy and inform patients about their upcoming procedures. “The models help ease patient anxiety,” he explains, noting that patients feel more confident and comfortable as he demystifies each part of the process.
Educational benefits

The time spent producing these scale models is not time wasted, it’s time learning. While preparing models for 3D printing, Dr. Schwenke and his team are able to learn more about patient aneurisms. “These models are extremely valuable to student doctors so that they can better understand how the blood flows through the arteries that connect the neck and the brain,” says Dr. Schwenke. And once printing starts, they’re free to continue seeing patients.
Before Dr. Schwenke developed this process, student doctors had to rely on visualizing these complex models primarily in their heads or with 2D representations. Now with the creation of these 3D printed models, student doctors can accelerate their learning path to becoming surgeons.

Though learning opportunities are reason enough to adopt this process, the benefits stretch beyond the classroom. Take cost, for instance. A generic aortic model costs $20,000 on average, and patient-specific models cost even more. Think about it: for the cost of a single generic model, you can stock an entire print lab to produce models in-house.
With this new process, patients are seen faster, surgeries become less risky, and costs are lowered. The best part, though? Dr. Schwenke and his team can save more lives than ever before.
What’s next for Dr. Schwenke’s team? “We’re hoping for new materials that are closer facsimiles to arterial tissue, for prints, which we can combine with robotic surgeries.” Sounds like the future of medical 3D printing will continue to be a bright one.
